Enhanced Point of Care Ultrasound Skills after additional instruction from simulated patients.

POCUS SP-Teacher poster
Ultrasound Localization to Resuscitate in Arrest (ULTRA) Research Program
RESEARCH AIMS: Chest compressions play a key role in the chain of survival in cardiac arrest (Sasson et al., 2010; Nichol et al., 2015; Kleinman et al., 2015). Compressions may prove more effective if rescuers could identify the area overlying the patients’ left ventricle, leading to direct its compression. We aim to determine if an area of compression over the left ventricle can be identified by either rapid sonographic localization or by a novel landmark-based approach. With initial results showing significant correlations for both sonographic and landmark-based approaches on volunteer patients, we intend to proceed with a two-pronged research program.

BACKGROUND: Survival from out-of-hospital cardiac arrest remains low, averaging 10% (Sasson et al., 2010; Nichol et al., 2015; Kleinman et al., 2015). Current guidelines advise compressions be done over the lower half of the sternum (Kleinmanet al., 2015); however, emerging evidence suggests that the current area of compression often results in aortic outflow obstruction (Pickard, Darby and Soar, 2006; Hwang et al., 2009; Cha et al., 2013; Shin, Rhee and Kim, 2007; Nestaaset al., 2016), potentially compromising effect. Compression directly over the left ventricle (LV) may improve pump effect (Rudikoff et al., 1980; Hwang et al., 2001; Georgiou, Papathanassoglou and Xanthos, 2014) and in one animal study (Anderson et al., 2017), was associated with increased return of spontaneous circulation. Furthermore, human studies involving the use of transesophageal echocardiography in arrest suggest that moving the area of compression based on scans during arrest can alleviate aortic outflow obstruction and improve LV compression (Zanatta, Benato and Cianci, 2015; Arntfield et al., 2016; Catena et al., 2019; Blaivas, 2008; Fair et al., 2018; Long et al., 2018). While these findings require further study, they do little to address the reality that rescuers attending out-of-hospital cardiac arrest will not have such devices available to them.
ABSTRACTS
P066: Ultrasound localization to resuscitate in arrest (ULTRA) Olszynski P, Woods R, Netherton S, Hussain Q, Blondeau B, Dunn S. Canadian J Emerg Med. 2019;21:0. [Google Scholar]
PEER REVIEWED PUBLICATIONS
- Olszynski PA, Bryce R, Hussain Q, et al. Use of a Simple Ultrasound Device to Identify the Optimal Area of Compression for Out-of-Hospital Cardiac Arrest. Cureus. 2021;13(1):e12785. Published 2021 Jan 19. doi:10.7759/cureus.12785
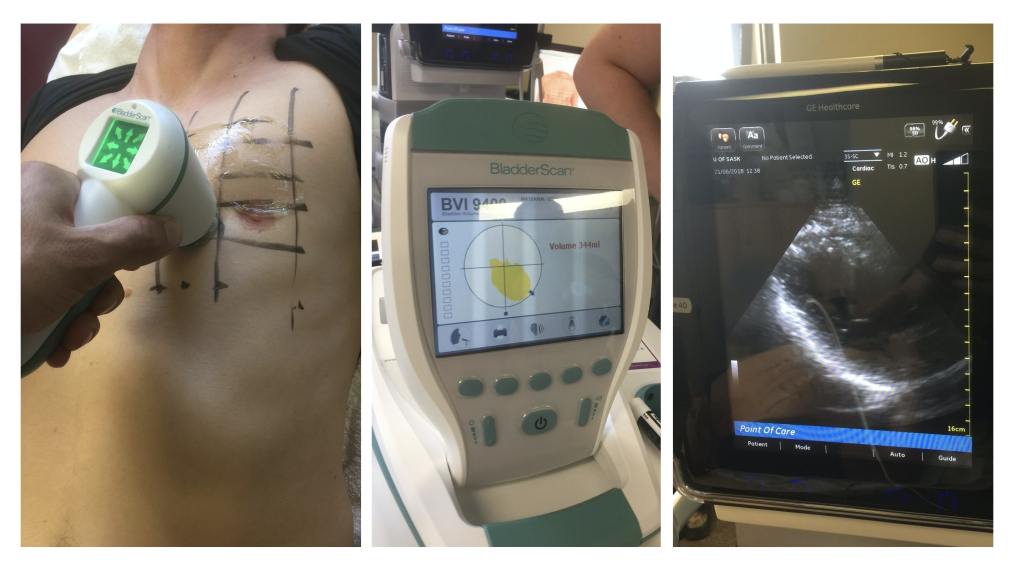
Conclusion: In this cross-sectional study, a simple ultrasound device (bladder scanner) was used to reliably localize the heart. In the healthy volunteers, the intercostal space of the largest scan volume was most often associated with the area overlying the long-axis view of the LV. This location, as identified through the scanner, represents a theoretically optimal area of compression.
Further investigation into rapid sonographic localization of the heart to guide the area of compression for OHCA is warranted.
2. Olszynski PA, Bryce R, Hussain Q, et al. A Novel Anatomic Landmark to Target the Left Ventricle During Chest Compressions in Cardiac Arrest. Cureus. 2021;13(3):e13652. Published 2021 Mar 2. doi:10.7759/cureus.13652

Conclusion: Utilizing ultrasound to map the position of the LV to the surface anatomy of our adult participants, we were able to identify an area of compression that may result in LV compression in most patients. Performing chest compressions over the left sternal border at the intersection of the inter-nipple line should be feasible for first responders and could optimize chest compression in cardiac arrest in a majority of patients.
3) Olszynski, P., Marshall, R.A., Olver, T.D. et al. Performance of an automated ultrasound device in identifying and tracing the heart in porcine cardiac arrest. Ultrasound J 14, 1 (2022). https://doi.org/10.1186/s13089-021-00251-5
https://theultrasoundjournal.springeropen.com/articles/10.1186/s13089-021-00251-5/figures/2
CONCLUSION: In this cross-sectional study, an automated ultrasound device (bladder scanner) was able to reliably identify and trace the borders of porcine hearts at the time of cardiac arrest. Bladder scanner performance was best during the initial arrest state and deteriorated significantly in late arrest likely due to low flow and clotting in the cardiac chambers. Further investigation into rapid sonographic localization of the heart to identify the area of LV compression in OHCA is warranted.
Further investigation is warranted to determine if the proposed area of LV compression is valid in a larger cohort of patients including those with cardiac and thoracic disease.
